Preclinical Study of Intraprostatic Ethanol Injection via a Microporous Needle: Correlation of Injected Volume and Lesion Size
Tyler Oe, BA1; Matthew Sommers, BA1; Benjamin King, MD1; Tarjei Bern Aaser, MD2; Eva Kildall Hejb�l, BSc2; Henrik Daa Schr�der, MD, PhD2; Mark Plante, MD1; Peter Zvara, MD; PhD2
1Larner College of Medicine at the University of Vermont, Burlington, VT; 2University of Southern Denmark, Odense, Denmark.
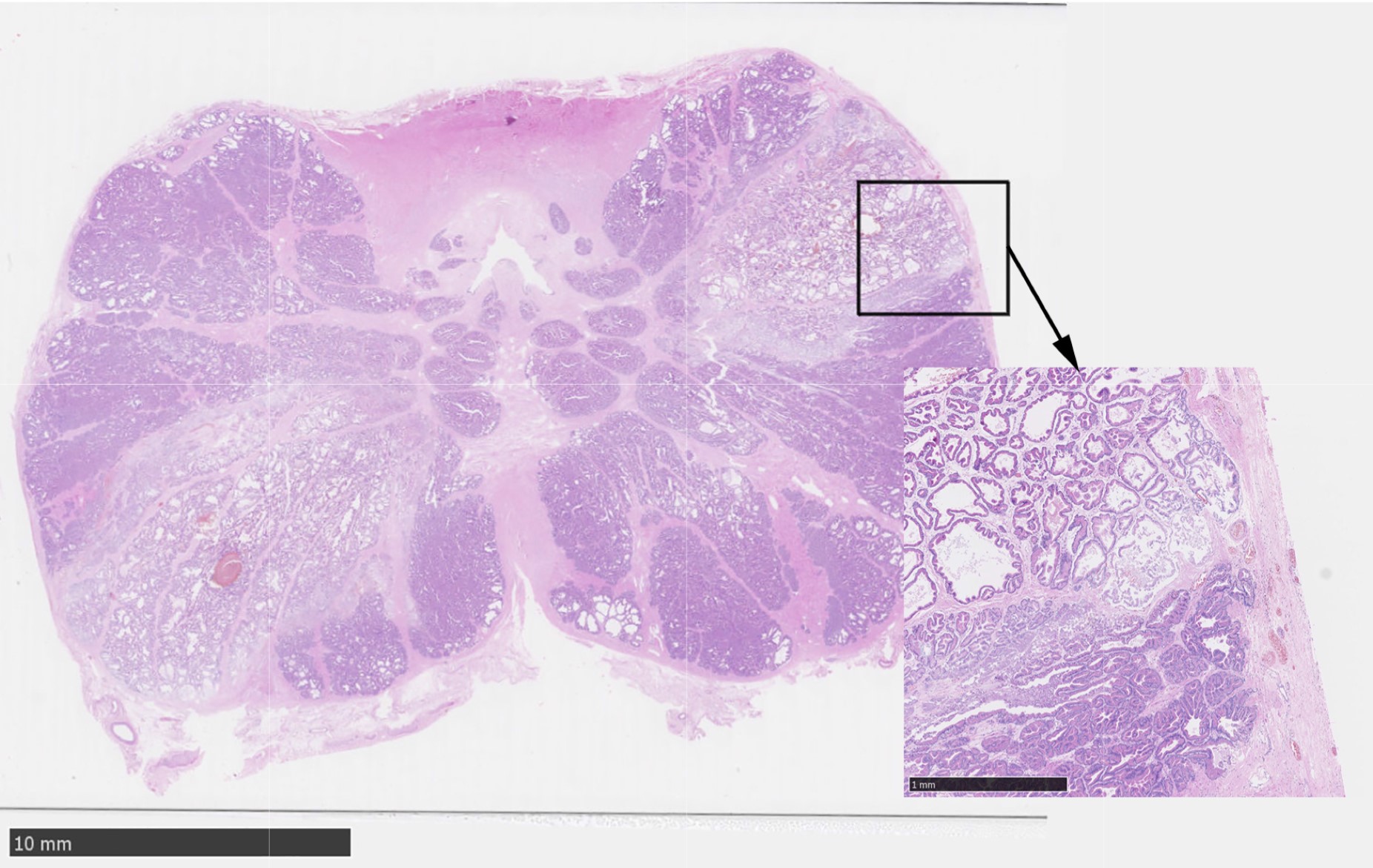
BACKGROUND: Prostate cancer (PCa) remains the most commonly diagnosed cancer and is the second leading cause of cancer death in men. Currently, treatment options for localized PCa lesions are limited to techniques involving periprostatic tissue damage causing significant adverse effects. With the guidance of novel imaging techniques, intraprostatic injection has potential to fill this gap as a minimally-invasive PCa therapy. We previously documented that intraprostatic anhydrous ethanol (EtOH) injection through a 1 cm microporous needle, ablated tissue, offered improved diffusion characteristics, and decreased backflow along the needle track when compared to a traditional needle. The objective of this study is to assess the properties of intraprostatic injection by calculating the lesion volumes, comparing lesion volumes with injection volumes, and generating precise 3D reconstructions of the prostate with the corresponding lesions. METHODS: Seven canine prostates were exposed by laparotomy and each prostate received EtOH injections of differing volumes into the right and left lobes. A 1 cm microporous needle was used to inject 0.5, 1.0, 1.5, or 2.0 mL of EtOH at a rate of 0.25 mL/min. Prostates were removed two hours post injection. 3 μm sections of prostatic tissue spaced 4 mm apart were processed with H&E for histological analysis. Stereo Investigator was used to outline the prostates and corresponding lesions. Cavalieri Estimator calculated the volume of the lesions and generated 3D representations of the prostate and lesions. RESULTS: Intraprostatic injections yielded oval lesions that were fully contained within the prostatic psueudocapsule. EtOH diffused throughout the glandular tissue and smooth muscle, resulting in glandular dilation, shrinkage of cell nuclei, and loss of visible nucleoli. The pseudocapsule remained intact and showed no sign of EtOH-mediated destruction. Injections of 0.5, 1.0, 1.5, and 2.0 mL yielded average lesion volumes of 208, 588, 791, and 1158 mm3, respectively. A regression analysis of the volume-necrosis relationship showed an R2 of 0.8493. CONCLUSIONS: In this study, we successfully injected seven canine prostates with EtOH and confirmed that intraprostatic injection with a micropourous needle ablates prostate tissue by inducing coagulative necrosis without backflow of EtOH along the needle track. Histological analysis of the prostates confirmed injections were confined to the prostate with no leakage of EtOH outside the prostatic pseudocapsule. Volume analysis confirmed that tissue ablation occurred in a reliably dose-dependent manner, highlighting the customizable nature of intraprostatic EtOH injection as a safe, reproducible, and cost-effective potential new PCa treatment method. 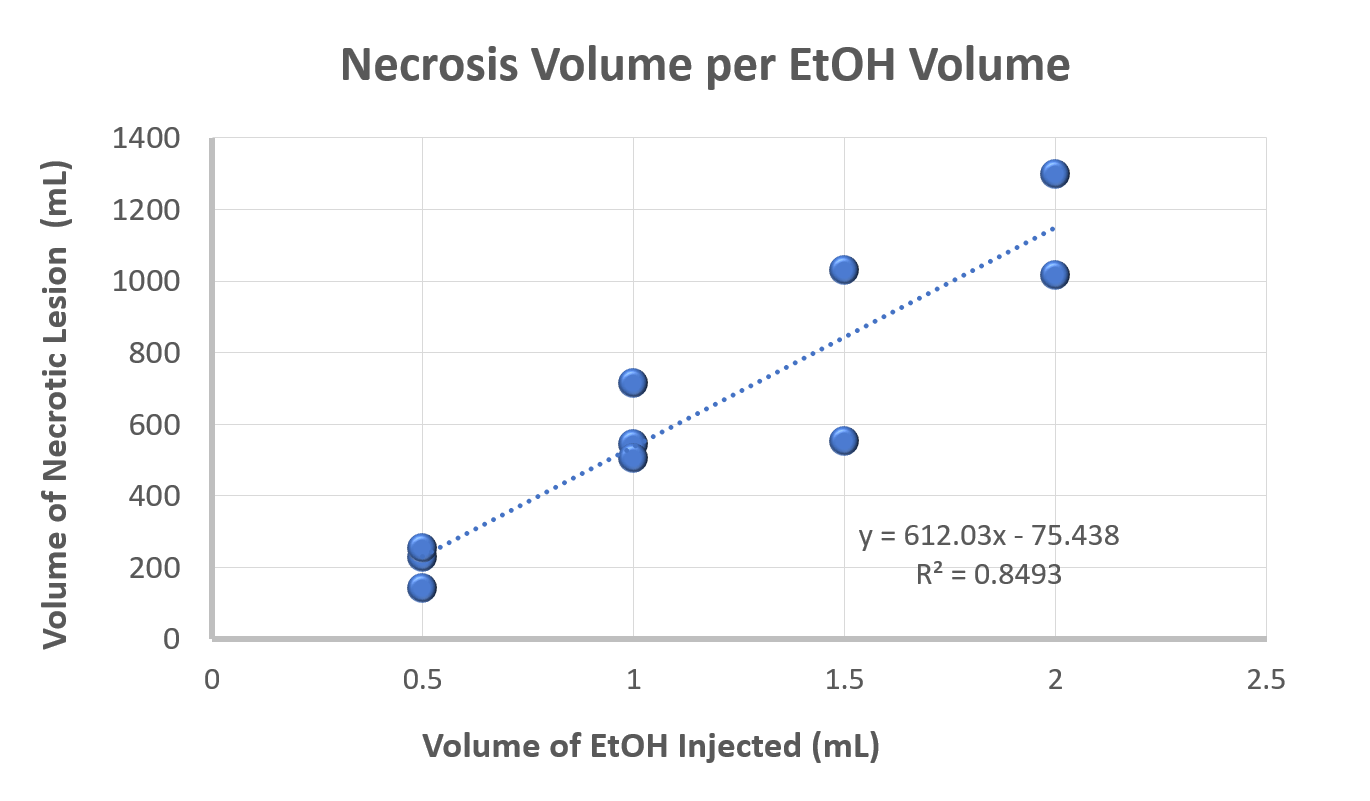
Back to 2018 Program
