Back to 2017 Program
Urethroplasty outcomes for an algorithmic approach for fossa navicularis urethral strictures
Mark Broadwin, BA, MS1, Alex J. Vanni, M.D.2.
1Tufts University School of Medicine, Boston, MA, USA, 2Lahey Hospital and Medical Center, Burlington, MA, USA.
Introduction:
Reconstruction of fossa navicularis (FN) strictures is difficult, requiring a multitude of reconstructive techniques to achieve both a normal cosmetic appearance and patent urethra. A combination of both 1 and 2 stage procedures using both buccal mucosa grafts (BMG) and fasciocutaneous flaps have been reported. Although there is no universally accepted technique, many prefer a 2 stage approach for FN urethral reconstruction. We have implemented a standardized algorithm for FN stricture reconstruction based on etiology, lumen size, and glans size to maximize the number of 1 stage reconstructions performed. The objective of our study was to evaluate the outcomes of this standardized approach.
Materials and Methods:
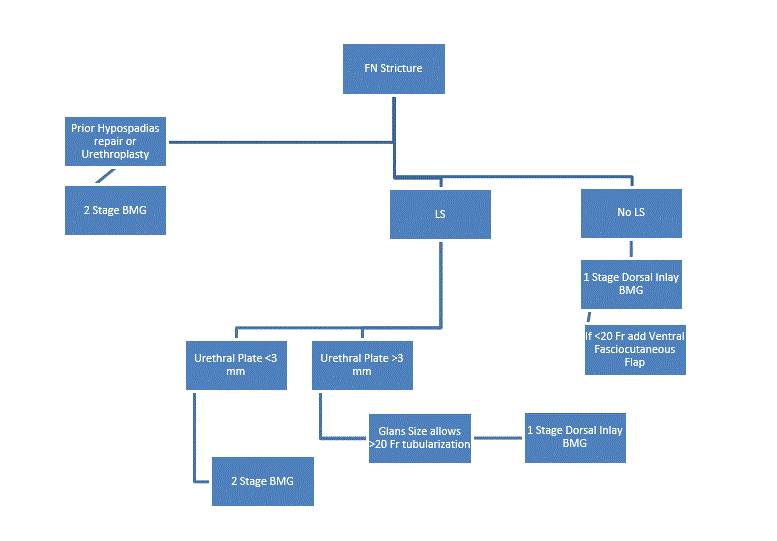
A retrospective review of a prospectively maintained urethral reconstruction database from 2011-2017 was performed. Patient demographics, stricture etiology and outcomes were recorded. Patients with isolated FN strictures undergoing urethroplasty via standardized operative algorithm were included for analysis (Figure 1). Patients with an isolated meatal stenosis, those undergoing a meatotomy or meatoplasty, or a penile stricture involving the fossa navicularis were excluded. Pre and postoperative assessment included questionnaires to assess sexual function and patient perception of genital function. Stricture recurrence was defined as the need for subsequent procedure.
Results:
A total of 460 patients were identified in the anterior urethroplasty database. 34 patients met inclusion criteria for analysis. 29% patients had LS, 6% had hypospadias, 44% were iatrogenic, and 9% were idiopathic. 18 (53%) patients underwent a one stage dorsal inlay BMG, 10 (29%) underwent a two stage repair with BMG, and 6 (18%) underwent a combined dorsal inlay and fasciocutaneous flap repair. 2 stage BMG repairs were performed in all hypospadias strictures, and in 50% of LS strictures.
At an average follow-up of 6.8 months there was one stricture recurrence.
Changes in average SHIM score were recorded with improvements seen in the dorsal inlay group (∆SHIM = +0.67), no change was noted in those undergoing two-stage repair (∆SHIM = 0), and a decreased average score was reported for those undergoing dorsal inlay and fasciocutaneous flap repair (∆SHIM = -3.5). All patients completing a postoperative satisfaction questionnaire were either “very satisfied” (67%) or “satisfied” (33%).
2 patients reported increased penile sensitivity following surgery (dorsal inlay, dorsal inlay + flap), while 3 patients reported a decreased penile sensitivity following surgery (dorsal inlay).
All patients state they would undergo the repair again given the chance. All but one dorsal inlay patient stated they would recommend urethroplasty to others with urethral stricture disease.
Conclusions:
An algorithmic approach to reconstruction of FN strictures demonstrates that the majority can be successfully reconstructed with a 1 stage procedure. 2 Stage procedures should be reserved for patients who are hypospadias repair failures or with obliterative lichen sclerosus strictures. Postoperative sexual function complaints are rare regardless of reconstruction technique.
Back to 2017 Program
|
|
|
|



